Reasons to choose Dr. Corrado
Philosophy
Dr. Corrado believes that every patient’s nose is unique, requiring an individualized approach towards every rhinoplasty. Each patient exhibits differences in nasal anatomy and structure. The qualities of the nasal skin, cartilage, and bone will all create different challenges which require a personalized surgical plan.
Form & Function
Many failed rhinoplasties are performed where the surgeons do not respect the functional aspects of the nose. In these cases, nasal collapse and difficulty breathing are very common. Dr. Corrado believes in not only providing the best cosmetic result for his patients but also delivering a nose that functions the same if not better than prior to surgery. Modern rhinoplasty surgery strives to strike a balance between nasal aesthetic form and nasal function.
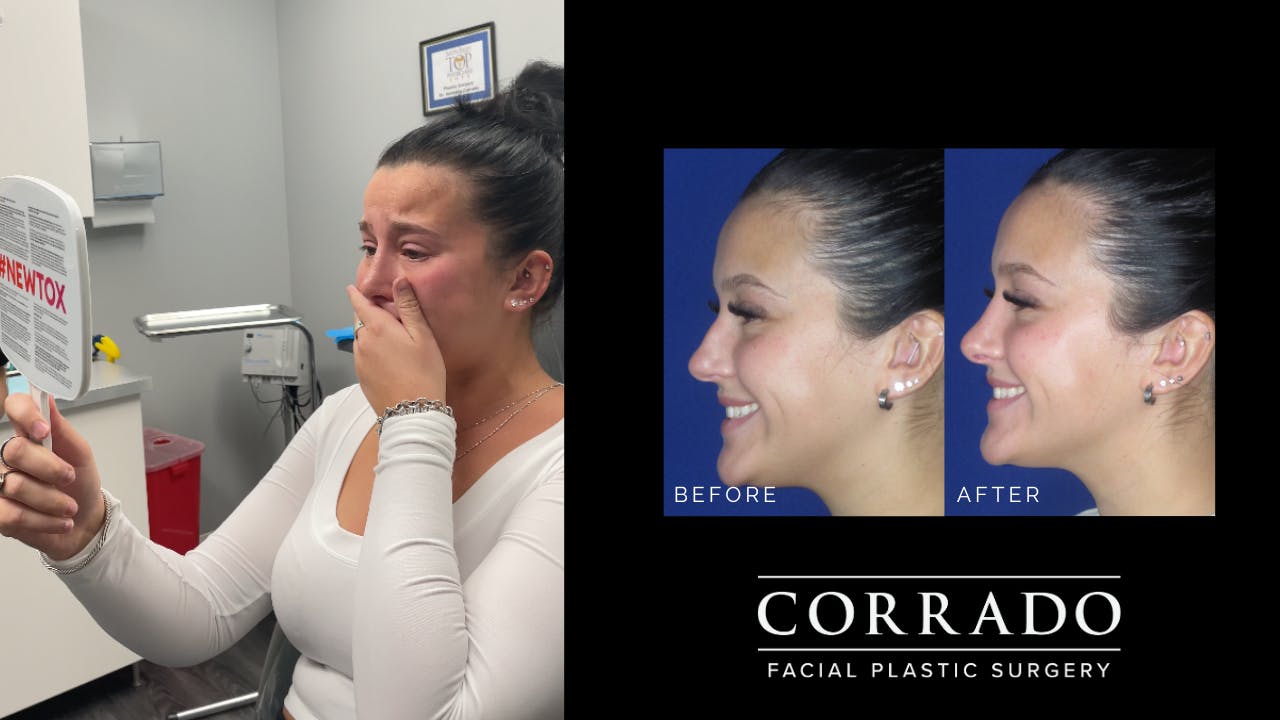
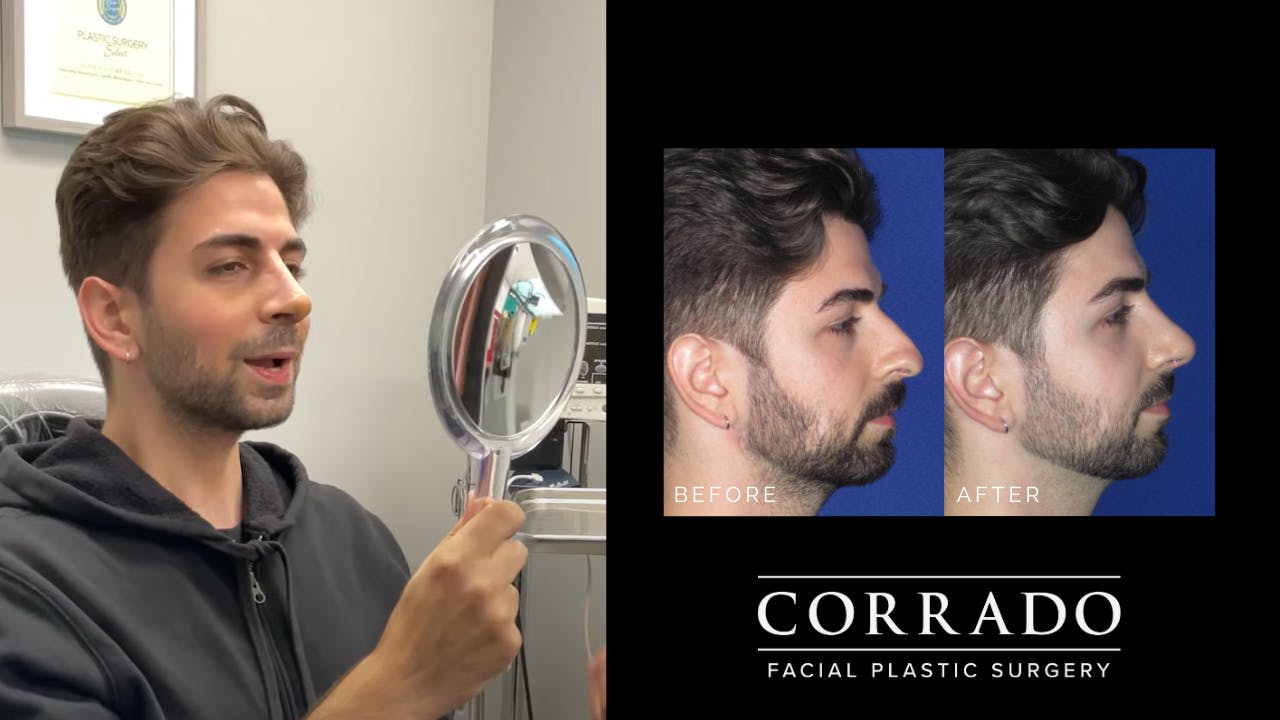
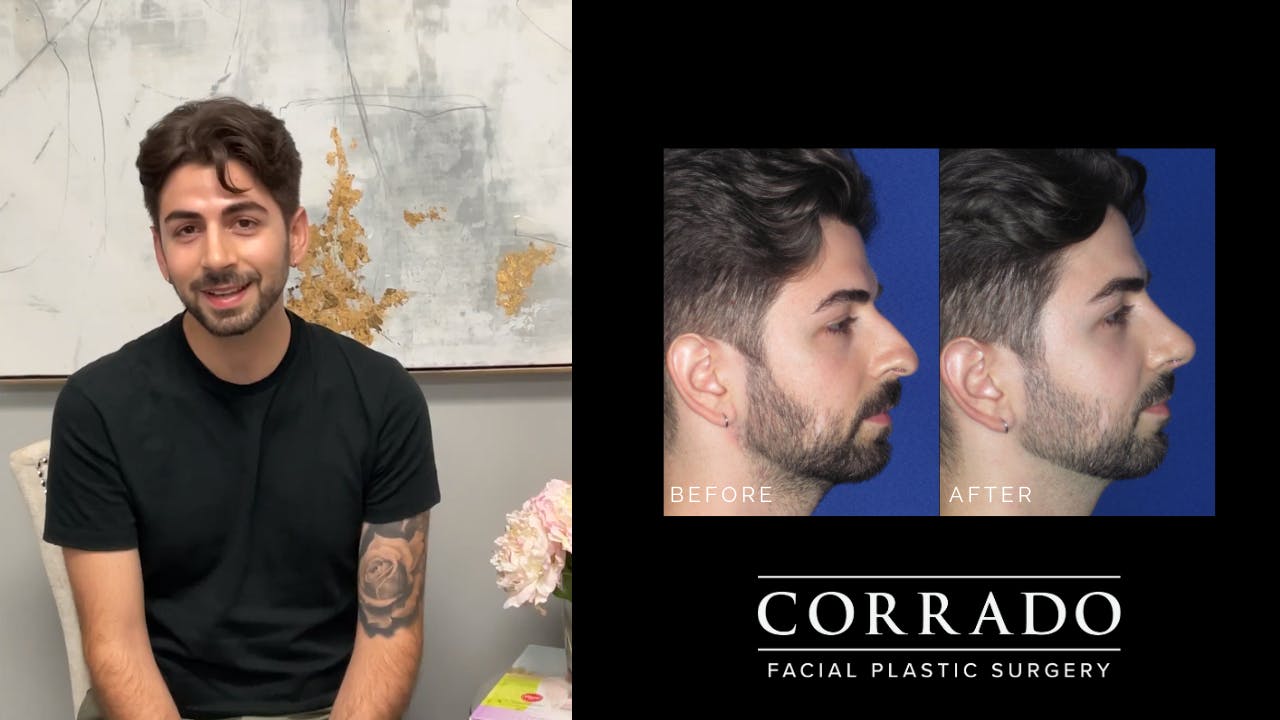
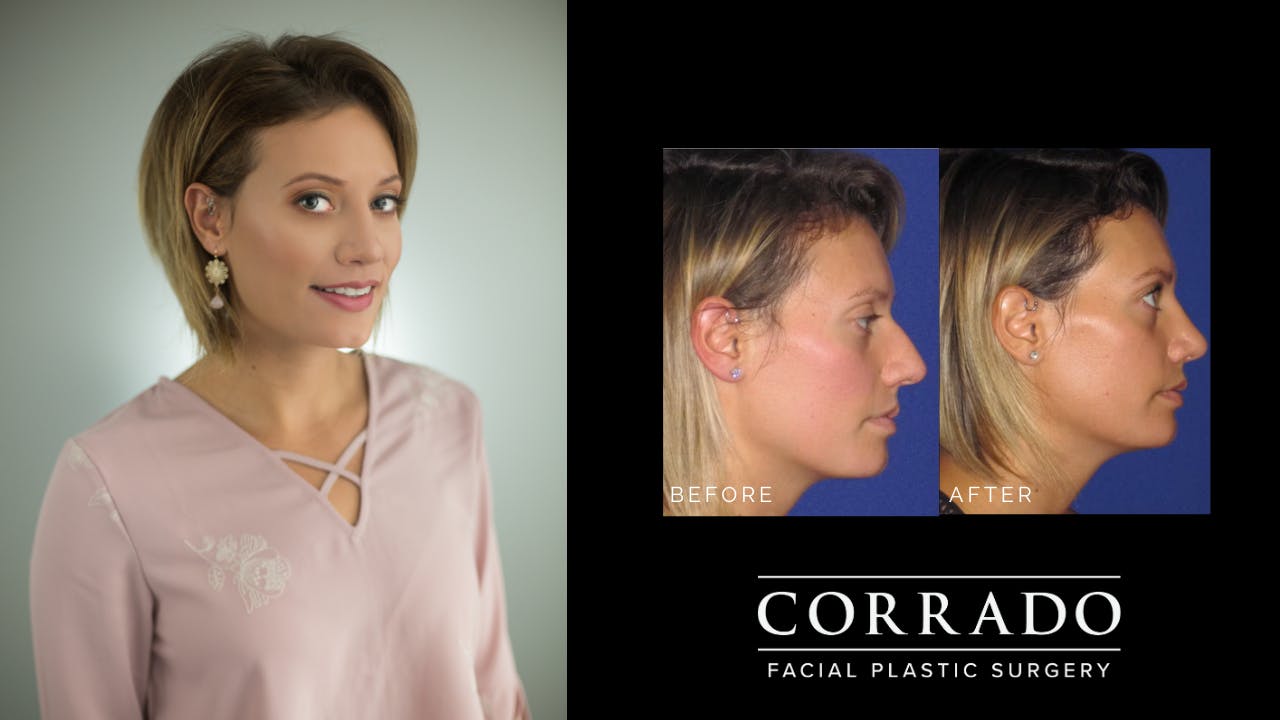
Natural Result
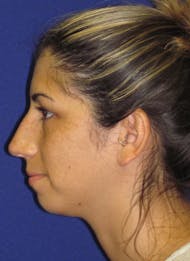
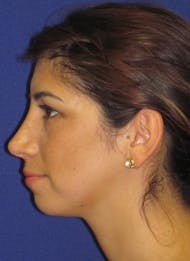
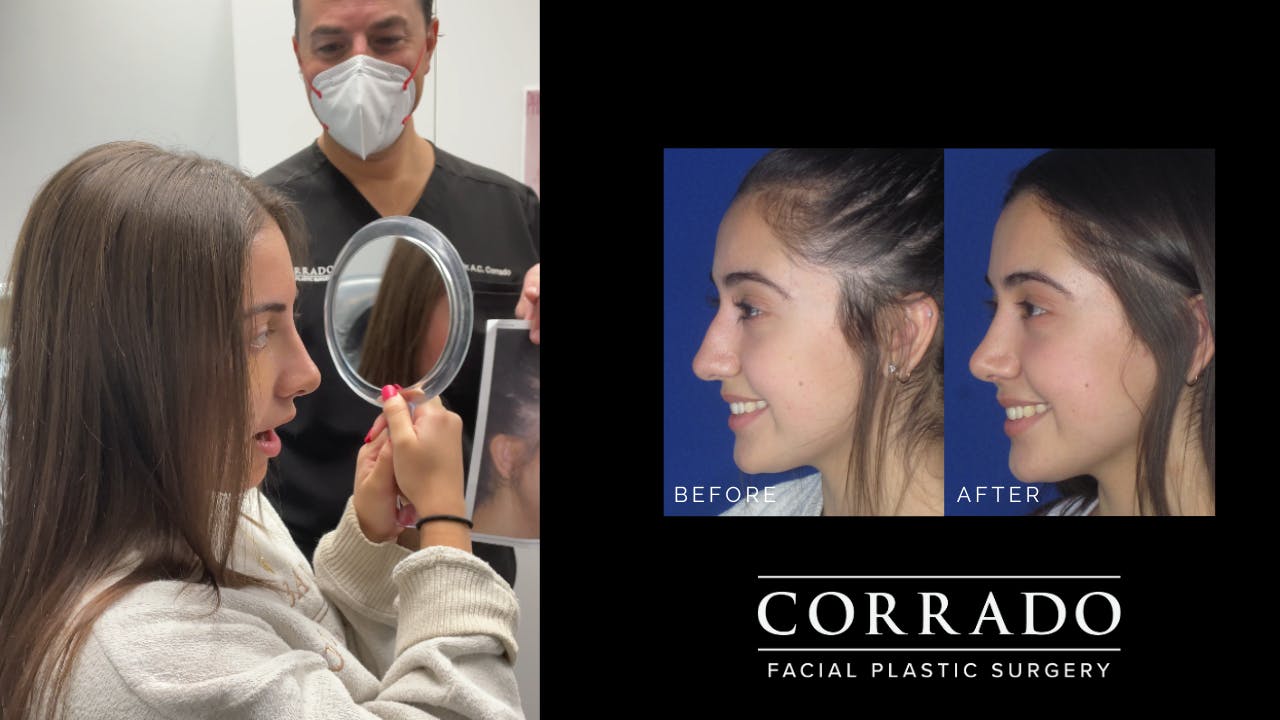
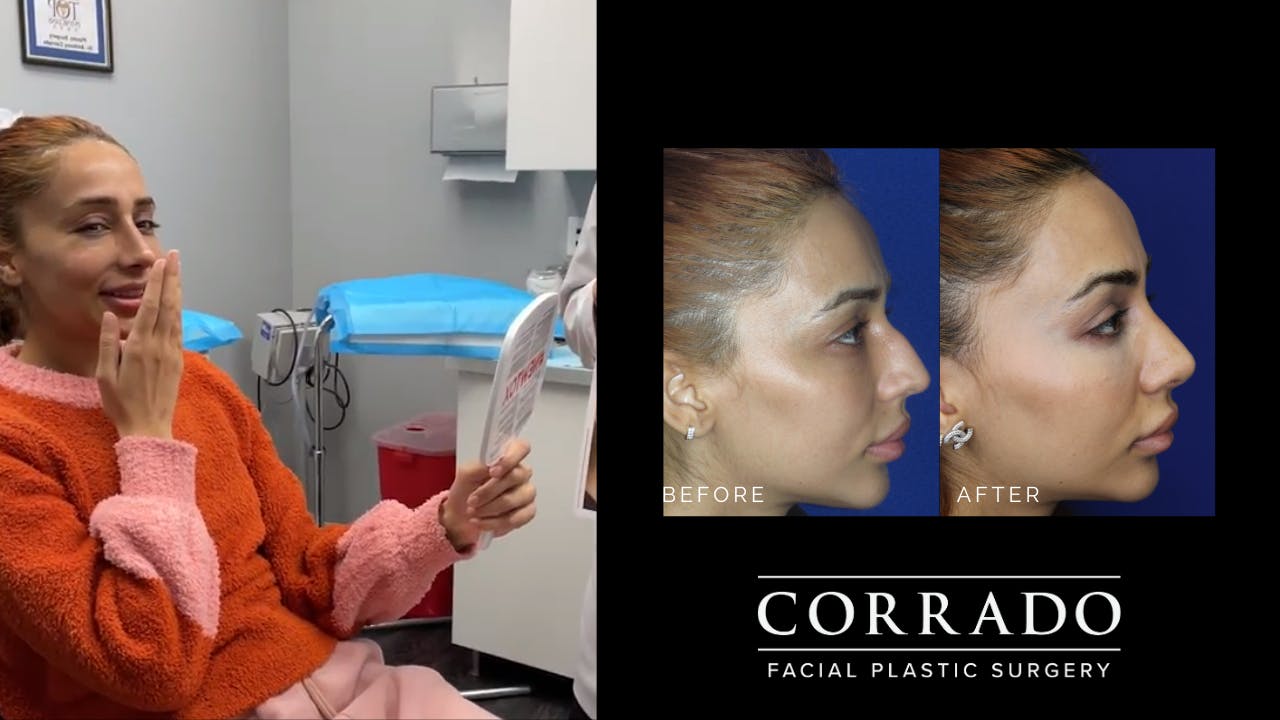
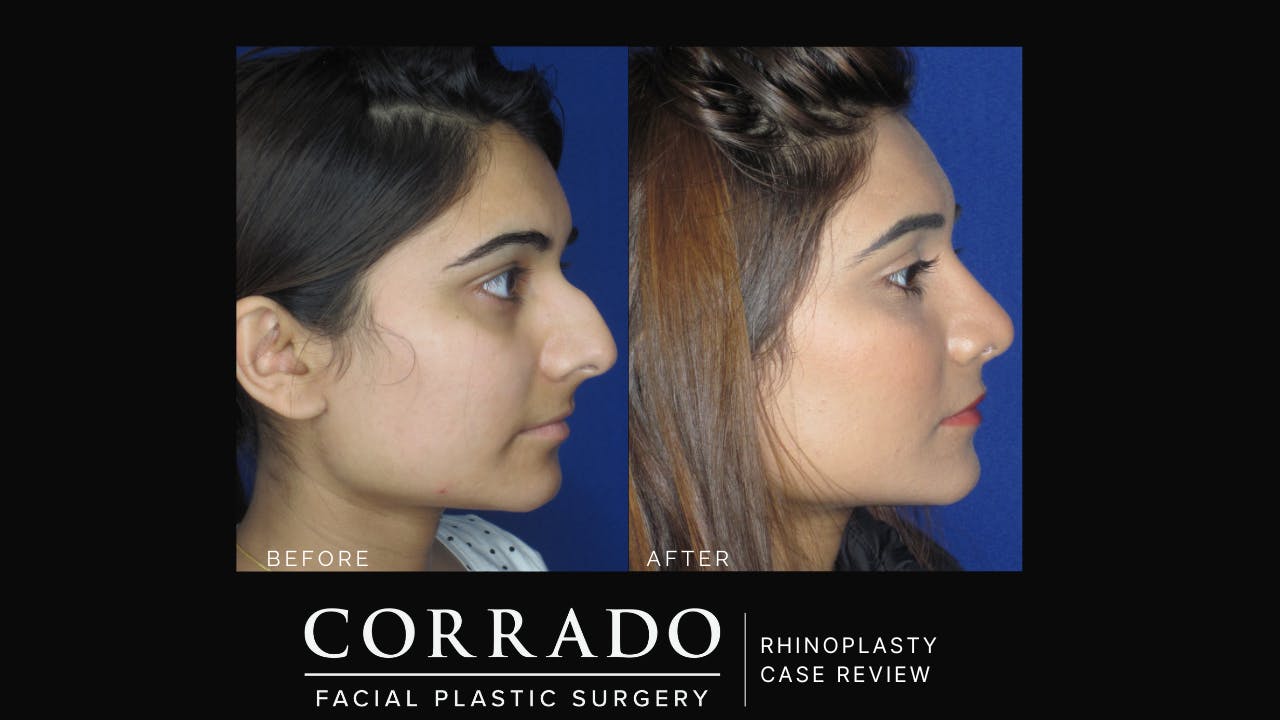
Dr. Corrado strives for natural-looking results without the tell-tale signs of “overdone” nasal surgery. Long gone are the overly pinched and scooped rhinoplasties of the ’90s. The “cookie cutter” approach is never used, and corners are never cut. Although it may have been easy to pick out patients who had “nose jobs” in the past, the modern belief in rhinoplasty is to create a nose that strikes a natural balance with the rest of the face. Patients from Philadelphia and across the country seek Dr. Corrado for a natural look—think noses with smooth lines and gentle contours. Dr. Corrado’s goal is to create a naturally beautiful result so that others will think you were just “lucky” to be born with such a great nose. Don’t worry, your secret is safe!